Findings and procedure details
We present two patients,
who were diagnosed in adulthood with primary hypoparathyroidism due to parathyroid hypoplasia,
coexisting calcifications of basal ganglia in the central nervous system and psychiatric disorders associated with 22q11.2DS.
The first patient,
a 32 year old man,
complained of residual schizophrenia which then transformed into severe catatonia after a tetany attack that first occurred during an increased physical activity.
The laboratory tests revealed hypoparathyroidism without any other clinical evidence of Di George syndrome.
Moreover,
micro deletion 22q11.2 was confirmed in the genetic test.
In addition,
significant improvement was observed after administration of calcium,
vitamin D and low phosphate diet.
The second patient,
a 37 year old man,
presented borderline behaviour and was admitted to the hospital after an episode of syncope and epilepsy.
Laboratory test revealed hypoparathyroidism together with profound hypocalcaemia.
Besides this no other clinical evidence of the Di George syndrome has been identified.
However,
genetic testing for micro deletion 22q11.2 has not been performed due to the lack of patient`s agreement.
Nevertheless,
after administration of calcium,
vitamin D,
and low phosphate diet no more epilepsy and syncope episodes were present.
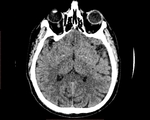
In both presented patients CT scan of the brain and scull and MRI of the brain demonstrate minor basal ganglia calcifications with the accompanying skull base deformation such as vertical clivus with reduced basal angle.
Minor basal ganglia calcifications,
also referred to as Fahr syndrome,
are considered as quite common,
incidental and idiopathic finding in elderly patients. If this sign is observed in younger patients,
pathological cause should be investigated. In patients with 22q11.2 deletion syndrome minor basal ganglia calcifications are a result of primary hypoparathyroidism [2].
Hypocalcemia can become a very serious condition,
and in some cases,
when serum calcium level is very low,
it might even be life-threatening,
so it is essential to make a proper diagnosis.
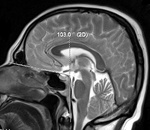
Skull base deformation is one of the most common anomaly in patients with 22q11.2 deletion syndrome.
In case of two patients presented we observed vertical clivus with reduction of basal angle.
In our measurement the angle was 112° in the first patient and 103° in the second one.
Angle less than 125° is considered as basilar kyphosis. However,
in literature a more often observed anomaly in patients with 22q11.2 deletion syndrome is platybasia,
with angle greater than 143° [3].
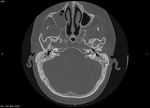
Another finding in one of our patients were hypoplastic mastoid processes.
It could be connected with other abnormalities in this region.
According to literature,
common anomalies in such patients are outer, middle and inner ear deformities ,
such as auditory canal stenosis,
abnormal malleus and incus,
dense stapes superstructure, abnormal orientation of stapes,
vestibule and lateral semicircular canal composed of a single cavity and wider vestibule [4].
In one case a small posterior fossa and cerebellum are seen. That was also described in some previous case reports and case series. In some cases cerebellum atrophy and reduction of cerebellar vermis hemisphere size were noticed.[1,2]
Both presented patients were diagnosed with primary hypoparathyroidism due to parathyroid hypoplasia and psychiatric disorders.
According to studies,
nearly 9-50% of 22q11.2DS reveal behavioral or psychiatric disorders during their life [1].
Probably one of the most common disorders is schizophrenia.
Comparing to general population,
those patients have almost 30-fold increased risk of this condition [6].
Although our patients didn’t have any brain midline developmental anomalies,
in some studies it was shown that in patients with schizophrenia and 22q11DS some midline developmental anomalies,
such as cavum septum pellucidum or cavum vergae,
were seen more often than in general population [1,2,6].
|
Imagining findings in 22q11.2 DS reported in literature.
|
|
Migration disorder
|
Polimycrogyria
Cortical dysplasia |
|
Developmental
midline abnormalities
|
Abnormalities of the septum pellucidum
Cavum vergae
Agenesis of the corpus callosum
Hypoplastic corpus callosum
Empty sella
Small pituitary gland
Ventricle enlargement
|
|
Cerebellar abnormalities
|
Hypoplastic cerebellar vermis
Cerebellar atrophy
|
|
Volume / size changes
|
Decrease in total brain volume
Increased size of caudate nucleus and insula
Decreased amygdale size
Microcephaly
|
|
Neurovascular findings
|
Abnormal cortical veins
Arterial abnormalities: hypoplastic internal carotid artery
|
|
Skull base abnormailites
|
Small posterior fossa
Short clivus
Prominent cisterna magna
Platybasia
Hypoplastic skull base
Small odontoid
|
|
Ear malformations
|
Outer ear: thickened tympanic membrane,
auditory canal stenosis
Middle ear: abnormal malleus and incus,
dense stapes superstructure,
abnormal orientation of stapes
Inner ear: incomplete partition type II with a normal vestibular aqueduct,
vestibule and lateral semicircular canal composed of single cavity,
to wide vestibule,
broadened lateral semicircular canal
|